How do we change a culture?
As a surgeon, there are critical defining steps in any procedure that I have to get right. This happens in the process of cultural change too. Let’s talk about this. I play the role of the catalyst, megaphone and signpost. I leverage the discussion around this issue and point the spotlight at certain things I believe to be the critical defining steps. I am just a megaphone.
Recently we have had a collision of topics around the culture of Medicine and Health Care. We have been speaking about: doctor suicides, mental health for doctors, mandatory reporting of doctors with mental health issues, toxic culture of medicine, inherent culture of bullying & harassment, unsafe working hours, burnout among doctors, resilience (or lack thereof), resilience programs, administrative overload, loss of job satisfaction, disillusioned doctors, commodification of doctors, McDonaldisation and industrialisation of Medicine, failure of Electronic Health Records, dehumanisation of doctors and other similar issues. These issues have been appearing on Australian TV programs, newspapers, radio, conferences and blogposts, but it’s a worldwide issue. There’s ample data to support the current negative decline in the Health of the Health Care Industry. It’s not a simple problem, and there isn’t a simple solution. We get that.
So how do we change a culture?
We start by changing the language. Cultures are build around language groups. We need to speak the right language in Medicine. For many of us, we can’t seem to articulate well enough the current problems with the health care industry. We know it has problems, but we can’t pinpoint the diagnosis and therefore we have no targeted effective treatment strategies. We call it burnout, but the solution is not simply more resilient programs. We know mental health is a factor, but the system itself is also a predisposing, precipitating and perpetuating factor. We know health administration, electronic health record and Key Performance Indicators are contributory factors in the disillusionment among doctors, but we also know that they are necessary tools in the context of Modern Medicine. How do we lift morale and efficiency at the same time? How do we reduce burnout, suicide and the stigma of mental health in medicine? How do we change the culture?
Let’s speak the right language together. We need to use a collective terminology and conceptual thinking to tackle these problems. Have you had that problem of trying to say something to another person but you can’t seem to articulate it well enough so you go looking for a card to express what you want to say? You find a card that encapsulates exactly what you really want to say. I had that moment when I was thinking about these issues. I saw this graph that switched on the light bulb in my head.
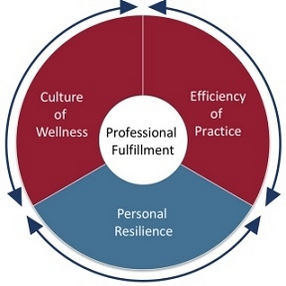
This is The Stanford Medicine Model for Physician Wellness. It’s beautiful, isn’t it? I saw it first on the webpage of the upcoming 2017 American Conference on Physician Health. The issues just became a bit clearer to me because the concept was given clear language and clarity of terminology in my mind. I think about it as the Tripod of Physician Wellness.
If we wanted to change the culture of the health care workers and health care industry, we need targeted approaches to these three problem areas. Focusing on one aspect (often just the individual resilience or mental health) alone become a victim-blaming exercise rather than a positive cultural change.
Personal Resilience
I know that this has become a word that carries bad connotations. Yes, there may be a resilience problem (although the evidence for this is generally anecdotal), but expecting resilience to simply happen without any training is like expecting a novice to handle the scalpel. It can hurt people. Resilience is a skill and a muscle. Training, coaching, exercises, tips, techniques and methods of resilience strengthening need to be taught. Like a muscle, it fatigues. You can’t expect any human doctor to be resilient 100% of the time all of the time in the context of oncalls, relocations, exams, research expectations, job applications and personal life challenges. You need to allow space and time for muscle rest. Debriefing, work-free spaces, staff rooms, help lines are good and necessary. As part of personal resilience is tackling the issue of mental health among doctors. We need to increase awareness, remove stigma, and dissolve any cultural and legal barriers to mental health support for doctors and clinicians. Both formal and informal suppport are critical to the development of mental health resilience and treatment. However, focusing only on resilience program is tunnel vision. Like the frog in the boiling water, you can’t merely teach the frog meditation and yoga to save itself. We need to do something about the boiling water as well. We need to address efficiency of practice and culture of wellness too.
Efficiency of practice
The side effect, or complication, of Modern Medicine is the increasing focus on efficiency systems at the expense of the humanity of clinicians. The Doctor can no longer just practice the Art of Medicine. They also have to practice the Business of Medicine. It frustrates me that the thing I love doing (seeing patients and operating on patients) is now recorded, measured, codified, benchmarked, audited and scrutinised by those who are not clinicians. Imagine asking an artist to paint faster and produce more paintings using the same amount of resources. Electronic health record has taken over the bulk of the burden of my day. Each week there seem to be new paperwork, protocols, guidelines and economic assessments on clinical activities. Click. Click. Click. The exponential increase of administrative officers in hospitals seem to slow things down for those down on the ground. We know from business research that with each additional layer of administration, there is loss of role clarity and loss of efficiency. This is the part where doctors just can’t do it on their own. We need strong involvement from hospital administrators. The problem, again, is the language. Health admins speak a different language. They want numerical results. We need to use their language to say that a mentally healthy doctor with a great job satisfaction is a doctor who is safe and efficient. The disillusioned doctor has a risk of over-investigating, under-treating or misdiagnosis. There is a business case to be made to invest in the health of doctors. Healthy doctors are good for patients and business. Revise the clunky electronic records that frustrate doctors. Improve the clerical support for clinics and operating rooms. Create safe rosters that avoid the existence of overworked clinicians who make mistakes. Remove the hospital hierarchy that puts Administrators at the top and clinicians down the bottom. Both admins and clinicians are on a level playing field working together for the patients. Admins as the support crew need to work together with clinicians to create an environment where clinical encounters are efficient for both patients and clinicians.
Culture of wellness
The hospital CEO need to have the same vested interest in the morale and health of clinicians as the Director of Physician Training. And this extends to non-clinicians as well. Patients and the Medical Institution benefit when every member of the health care team plays at their best. This include doctors, nurses, physiotherapists, speech pathologists, pharmacists, secretaries, biomedical engineers, janitors, etc. For it to permeate the institution, a Culture of Wellness begins at the top. Use the business language. What if staff wellness is a KPI for every hospital leader? What if a Staff Wellness Officer is appointed to ensure that targets are met? Just like blood pressure and temperature measurements, there are validated measures available that is applicable to track the health of an institution. What if the KPI for every CEO, CMO, Heads of Units, and Director of Division include the percentage improvement in Staff Burnout Scores or Leadership Scores? Make it a regular Grand Round topic, Audit Measure and Business Agenda.
There is an ethical, clinical and business case to be made to invest in the health of health care workers and the culture of health care. A healthy clinician is safe for the patient and good for the organisation. Addressing the Tripod of personal resilience, efficiency of practice and culture of wellness require courageous leadership and persistent grassroots momentum.
To change the culture, we must begin with changing the language. If we share the same concept, terminology and language, we can begin to talk about the right solutions with those who speak a different language (business, accounting, politics, ect). Speak to your supervisor or leaders. Let them know that the hospital stands or falls on this tripod. Help them direct their interventions around this tripod.
One last thing. If you would like a practical solutions-oriented published paper on this issue, please begin with this paper. I highly recommend this article as a starting point for anyone who work in health care.
Tait D. Shanafelt, MD, and John H. Noseworthy, MD, CEO. Executive Leadership and Physician Well-being: Nine Organizational Strategies to Promote Engagement and Reduce Burnout. Mayo Clin Proc. 2017;92(1):129-146

